WHAT IS OCD?
OCD: A LIFE-LONG BATTLE
1.5% of women and 1.0% of men worldwide suffer from OCD, a chromic neurodevelopmental anxiety disorder characterized by recurring, intrusive thoughts or images that cause extreme distress and anxiety – and the compulsive need to carry out repetitive, ritual acts to reduce that anxiety.
The WHO lists anxiety disorders, including OCD, as the sixth largest contributor to non-fatal health loss globally. Currently 9.45 million people live with moderate or severe OCD in Europe, the US, Japan and the UK.
A safe, fully effective pharmaceutical therapy still does not exist.
STIGMA, SECRECY, SEVERITY
Despite being so prevalent, the underlying neurological and hormonal mechanisms that cause OCD remain poorly understood. Current front-line treatment is demanding, arduous, costly and time-consuming. Recidivism is high. Of people diagnosed with OCD:
- 96% suffer from moderate to severe versions
- 50%+ experience impairment so serious they are unable to lead normal lives
- 40–50% remain resistant to current treatments
UNMET NEED, NEW DEVELOPMENTS
There is no safe, highly efficacious pharma medication for OCD, despite 50% of diagnosed patients being seriously impaired and unable to lead uninterrupted lives.
SSRIs have an overall efficacy of < 50%. They can be effective at reducing OCD anxiety, but they fail to treat the compulsive mechanism in OCD.
The lack of pharmaceutical options can lead to some physicians prescribing off-label medication with serious side effects (from second-line central nervous treatments like atypical neuroleptics or antipsychotics like Haloperidol).
FRONT-LINE TREATMENT
ALLOPREGNANOLONE: THE KEY TO COMPULSION?
A key factor in the lack of effective pharma therapy is the absence of a treatment that targets the compulsive mechanisminherent in OCD. The obsessive fear and anxiety element can be reduced somewhat through SSRIs. Yet that can only ever be half the story for a condition driven by two symbiotic motors – obsession and compulsion.
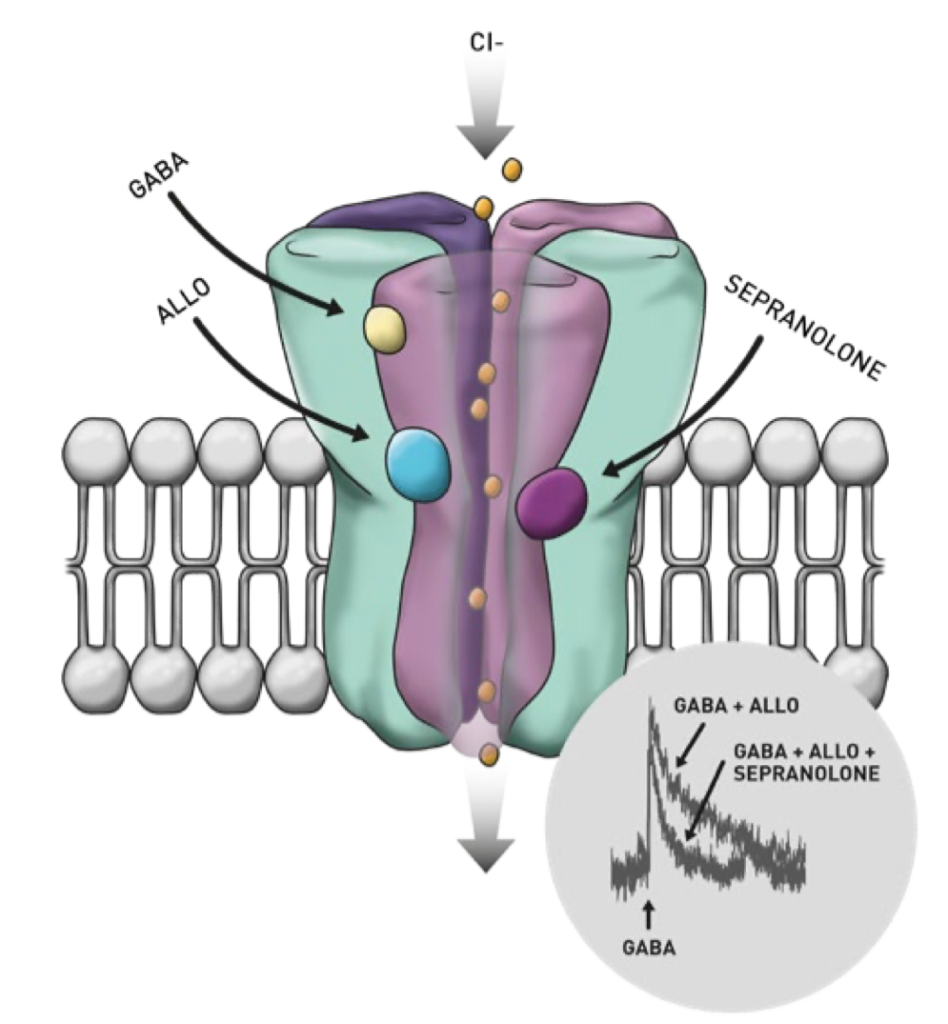
New research is now pointing towards the role of one of the brain’s most potent neurotransmitters – Allopregnanolone – in triggering compulsion.
And a treatment that modulates and inhibits the negative effects of this substance already exists…